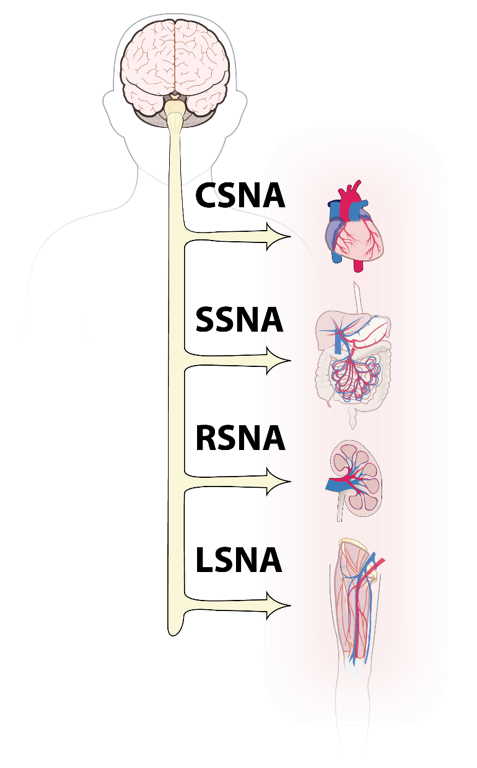
Is now clear that hypertension is associated with an increase in sympathetic nervous system (SNA) activity. Current pharmacological treatments for hypertension block global SNA and, although this is effective, these therapies also have numerous unwanted side effects. We are testing the hypothesis that hypertension is associated with a disease specific sympathetic signature such that sympathetic nerve activity is preferentially increased to specific vascular beds. If this is true, then targeted ablation of these peripheral pathways may be a superior therapy for treatment of hypertension. Our current studies are focused on the sympathetic nerves to the kidneys and splanchnic organs in the pathogenesis and maintenance of hypertension. This work has important clinical application in light of recent clinical trials with catheter based renal nerve ablation to treat drug resistant hypertension in humans.
____________________________________________________________
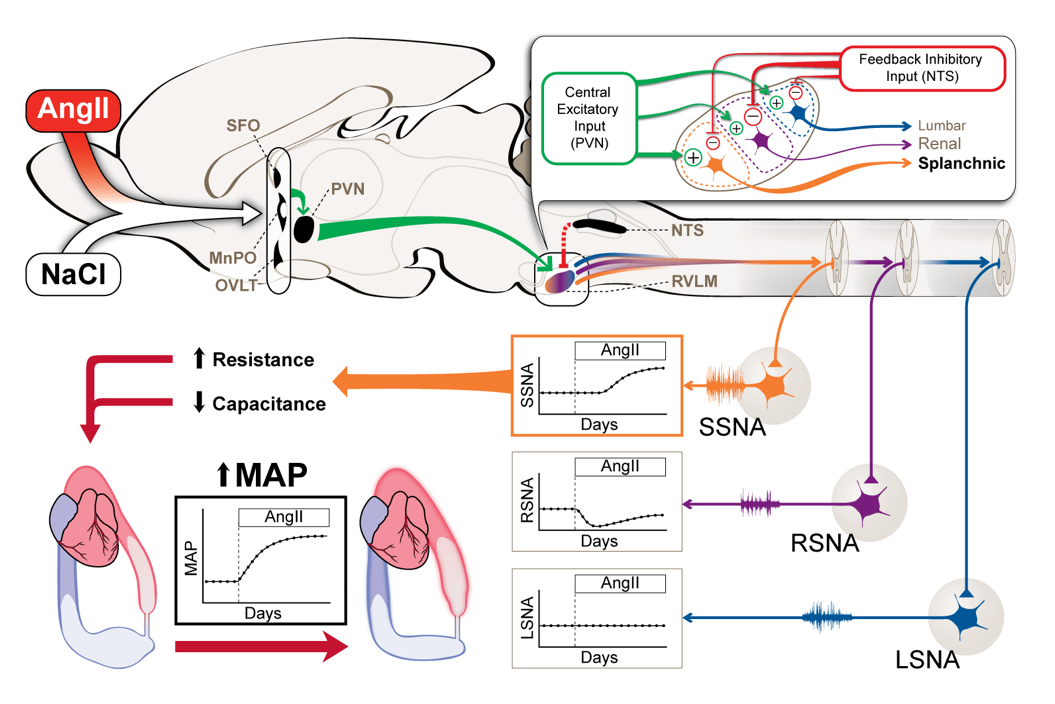
The figure below summarizes studies from our group in which we established the sympathetic signature of hypertension induced by chronic administration of angiotensin II (AngII) combined with a high salt diet (see J. Osborn, M. Kuroki and G. Fink, Current Hypertension Reports, 2011). This model is characterized by a chronic decrease in renal sympathetic nerve activity (RSNA), no change in lumbar SNA (LSNA) and an increase in splanchnic SNA (SSNA). Although the mechanisms mediating this differential pattern of SNA are still under investigation, this indicates that therapies targeting only SNA to the splanchnic circulation would be an effective treatment for hypertension that is driven by these inputs to the brain.